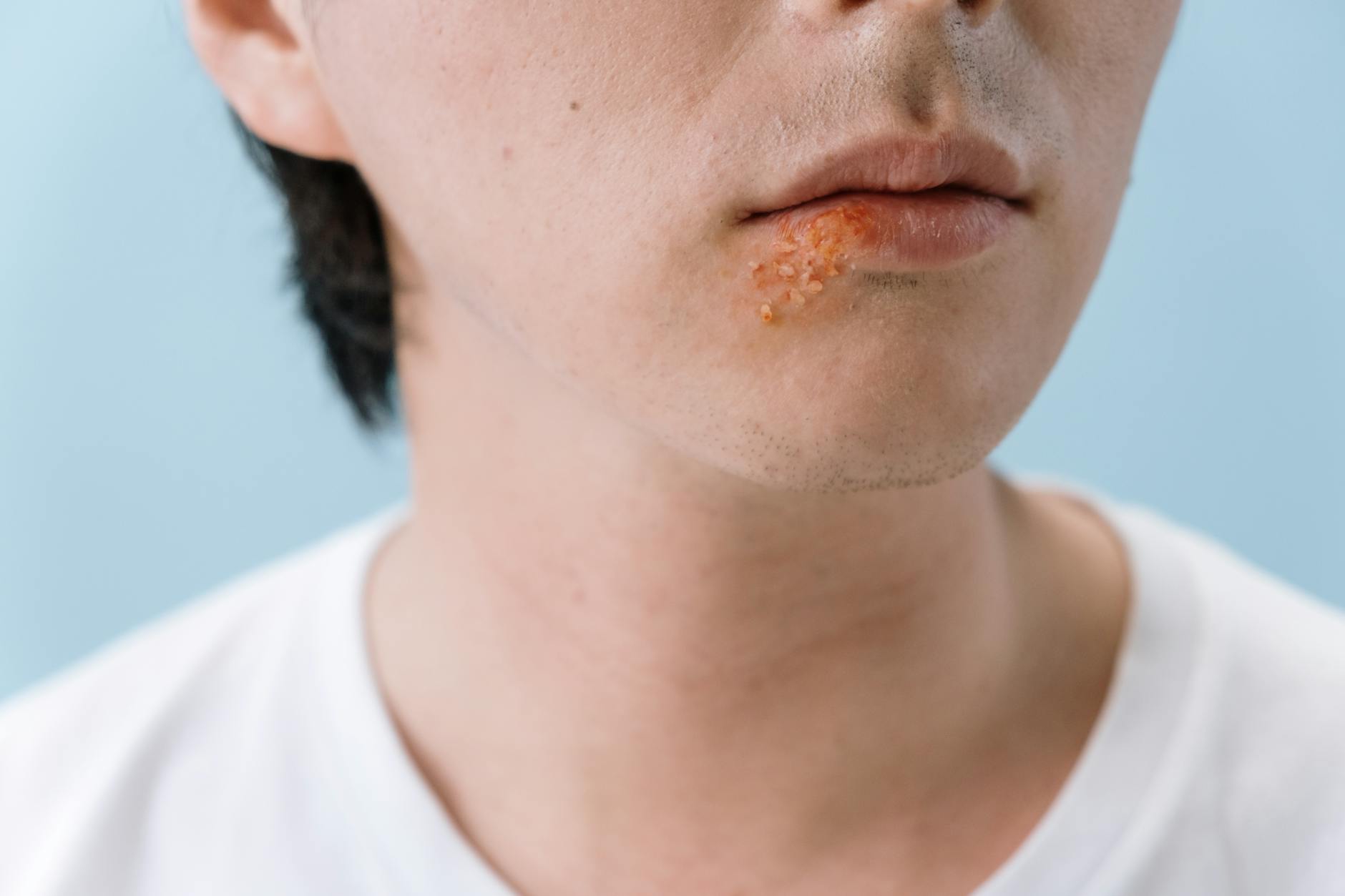
Sweet syndrome, also known as acute febrile neutrophilic dermatosis, is a rare inflammatory skin condition that can appear suddenly and dramatically. Though it affects people of all ages, it most commonly strikes women between 30 and 60 years old. Understanding this condition is essential because its symptoms can mimic infections or other serious diseases, making awareness a critical first step toward proper diagnosis and relief.
1. It Has Nothing to Do With Sugar or Sweetness
Despite its name, sweet syndrome has no connection to sugar, candy, or anything sweet. The condition was named after Dr. Robert Douglas Sweet, the British dermatologist who first described it in 1964. He documented a group of women who developed painful red skin lesions along with fever and elevated white blood cell counts. The name stuck, but it often causes confusion among patients hearing the diagnosis for the first time. If your doctor mentions sweet syndrome, know that it refers to a specific pattern of skin inflammation, not a dietary condition. Understanding the origin of the name can help ease the initial surprise of diagnosis.
2. Painful Skin Plaques Are the Hallmark Symptom
The most recognizable sign of sweet syndrome is the sudden eruption of tender, red or violet-colored plaques on the skin. These raised lesions typically appear on the arms, neck, face, or trunk. According to research published in PubMed, sweet syndrome presents with sudden tender plaques often accompanied by fever and joint pain. Unlike a simple rash, these plaques feel firm and are genuinely painful to the touch. They may also develop a bumpy or blistered surface that looks alarming. If you notice rapidly developing painful skin lesions paired with fever, seek medical attention promptly.
3. Fever and Fatigue Often Accompany the Skin Lesions
Sweet syndrome is more than just a skin problem. Most patients experience fever, fatigue, and a general feeling of being unwell alongside their skin lesions. Joint pain and muscle aches are also frequently reported. These systemic symptoms occur because the condition involves widespread inflammation throughout the body, not just in the skin. The combination of fever and dramatic skin changes is actually what helps doctors distinguish sweet syndrome from other dermatological conditions. Paying attention to these accompanying symptoms and reporting them to your doctor can speed up the diagnostic process.
4. Neutrophils Play a Central Role in the Disease
At the microscopic level, sweet syndrome is defined by a dense infiltration of neutrophils into the skin. Neutrophils are white blood cells that normally fight infections. In sweet syndrome, however, they flood into the skin tissue without any infection present. As noted in a PubMed review, the condition involves a hypersensitivity reaction driven by cytokines and neutrophil infiltration. This is why it is formally classified as a neutrophilic dermatosis. A skin biopsy revealing this neutrophil pattern is one of the key diagnostic criteria your dermatologist will look for.
5. There Are Three Distinct Types of Sweet Syndrome
Clinicians classify sweet syndrome into three categories based on its underlying cause. Classical or idiopathic sweet syndrome accounts for the majority of cases and has no clearly identifiable trigger. Malignancy-associated sweet syndrome occurs in patients with an underlying cancer, most commonly blood cancers like leukemia. Drug-induced sweet syndrome develops as a reaction to certain medications, including granulocyte colony-stimulating factor and some antibiotics. Knowing which type you have matters greatly because it shapes the treatment plan and determines whether further testing for hidden conditions is necessary.
6. It Can Signal an Underlying Malignancy
One of the most important reasons doctors take sweet syndrome seriously is its association with cancer. Research from a review of 48 Mayo Clinic cases found notable associations between sweet syndrome and hematologic or internal malignancies. Leukemia, lymphoma, and myelodysplastic syndromes are among the most commonly linked cancers. This does not mean everyone with sweet syndrome has cancer. However, doctors will often run blood tests and additional screenings to rule out malignancy, especially in older patients or those with atypical presentations. Early detection of any underlying condition leads to better outcomes.
7. Certain Medications Can Trigger It
Drug-induced sweet syndrome is a recognized subtype that develops after exposure to specific medications. The most commonly implicated drug is granulocyte colony-stimulating factor, used to boost white blood cell counts in cancer patients. Certain antibiotics, oral contraceptives, and nonsteroidal anti-inflammatory drugs have also been reported as triggers. Symptoms usually appear days to weeks after starting the offending medication. The good news is that drug-induced cases often resolve once the medication is discontinued. Always inform your doctor about every medication you take if you develop unexplained skin lesions and fever.
8. Corticosteroids Are the First-Line Treatment
The standard treatment for sweet syndrome is systemic corticosteroids, most commonly prednisone. As highlighted in clinical evidence from PubMed, corticosteroids remain the first-line therapy for this condition. Most patients experience rapid improvement within days of starting treatment. The skin lesions begin to flatten, pain decreases, and fever subsides. However, tapering the medication too quickly can lead to recurrence. Your doctor will typically design a gradual tapering schedule over several weeks. Following the prescribed timeline closely is one of the most important things you can do to prevent flare-ups.
9. Alternative Treatments Exist for Those Who Cannot Take Steroids
Not everyone can tolerate corticosteroids due to side effects like blood sugar spikes, weight gain, or bone thinning. Fortunately, several alternative therapies have shown promise. Colchicine, a medication originally used for gout, is frequently used as a steroid-sparing option. Potassium iodide and dapsone are other alternatives that dermatologists may consider. In milder cases, potent topical corticosteroids applied directly to the lesions can provide relief without systemic side effects. Discuss your medical history and concerns openly with your doctor so they can tailor a treatment plan that works safely for you.
10. Recurrence Is Common But Manageable
One frustrating aspect of sweet syndrome is its tendency to recur. Studies suggest that roughly one-third of patients experience at least one recurrence after their initial episode. Flare-ups may happen weeks, months, or even years later. Recurrence is especially common in patients with underlying conditions that remain active, such as inflammatory bowel disease or a persistent malignancy. The reassuring news is that each recurrence typically responds well to the same treatments that worked before. Staying in regular contact with your dermatologist and reporting new symptoms early can help manage recurrences effectively before they become severe.
Sweet syndrome may be rare, but its sudden and dramatic symptoms make it a condition worth understanding. Whether you or someone you love is dealing with it, knowing the facts empowers better conversations with healthcare providers. If you notice painful skin plaques, unexplained fever, or joint pain, schedule a dermatology appointment as soon as possible for proper evaluation.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making health decisions.