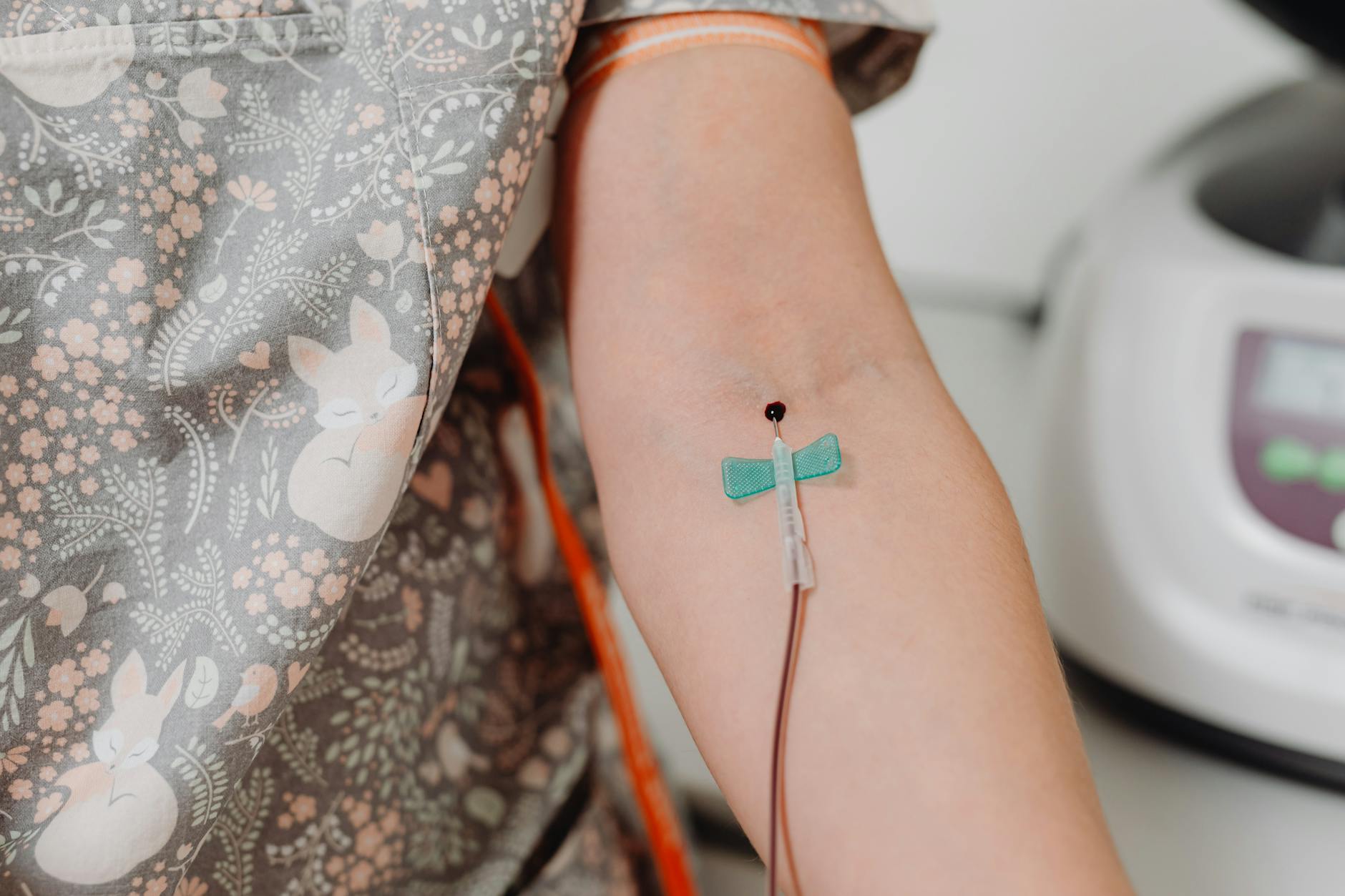
Phlebitis — inflammation of a vein — is one of the most common complications of intravenous therapy and can also occur on its own. It affects people of all ages, though certain groups face a higher risk depending on their health status and medical history. Understanding the warning signs and risk factors can help you take action early and avoid more serious complications like blood clots.
1. Phlebitis Is Vein Inflammation With Multiple Causes
At its core, phlebitis simply means that a vein has become inflamed. This can happen for several reasons. Trauma to the vein wall, infection, or irritation from chemicals like medications can all trigger it. The condition most often affects superficial veins close to the skin’s surface, particularly in the legs and arms. When it involves deeper veins, it becomes a more serious concern known as deep vein thrombophlebitis. If you notice unusual tenderness along a visible vein, that is a signal worth paying attention to.
2. Redness and Warmth Are Early Warning Signs
One of the first things people notice with phlebitis is a streak of redness along the path of a vein. The skin over the affected area often feels warm to the touch. Research emphasizes that signs like pain and redness should be assessed using systematic scales, and severity-based treatment should follow. These visual cues are your body’s way of signaling inflammation. If redness spreads or is accompanied by fever, contact your doctor right away rather than waiting to see if it resolves on its own.
3. IV Catheters Are a Leading Trigger
Peripheral intravenous catheters are among the most common causes of phlebitis in hospital settings. The catheter can irritate the inner lining of the vein, sparking inflammation. A large-scale study found that phlebitis incidence in Spanish hospitals exceeds recommended levels, with independent risk factors including higher numbers of infused medications and longer dwell time. If you or a loved one has an IV line in place, monitoring the insertion site daily can help catch problems early.
4. Pain and Tenderness Often Follow a Visible Pattern
Phlebitis pain is not random. It typically follows the line of the inflamed vein, creating a cord-like area of tenderness under the skin. The discomfort can range from mild soreness to significant pain that worsens with touch or movement. Some people also experience a slight throbbing sensation. Unlike muscle pain, this tenderness has a very linear path. Gentle elevation of the affected limb and applying a warm compress can often help ease discomfort while you await medical evaluation.
5. Certain People Face a Higher Risk
Not everyone is equally likely to develop phlebitis. Clinical evidence shows that older adults, women, and people with limited mobility face elevated risk. Obesity, smoking, and a history of varicose veins also increase vulnerability. Individuals taking hormonal medications like oral contraceptives may see higher rates as well. Research confirms that female sex and older age are independent predictors of phlebitis. If you fall into any of these categories, being proactive about vein health is especially important.
6. There Are Three Distinct Types
Phlebitis is not a one-size-fits-all condition. Mechanical phlebitis results from physical irritation, often caused by a catheter rubbing against the vein wall. Chemical phlebitis occurs when medications or IV fluids irritate the vein lining. Bacterial phlebitis happens when microorganisms enter through a break in the skin. Each type has slightly different prevention strategies, which is why healthcare teams focus on proper catheter placement, medication dilution, and sterile technique. Knowing which type is involved helps guide the most effective treatment.
7. Catheter Size and Placement Matter More Than You Think
The details of how an IV line is placed can significantly influence phlebitis risk. Research suggests that catheter gauge, insertion site, and catheterization duration are highly associated with phlebitis occurrence, though specific comparisons have not always reached statistical significance in meta-analyses. Generally, using the smallest catheter that works for the treatment and placing it in a larger vein can reduce irritation. Asking your nurse about these factors during hospitalization is a reasonable and empowering step.
8. Superficial Phlebitis Usually Resolves Well
The good news is that superficial phlebitis — affecting veins near the skin — typically improves within one to two weeks with conservative care. Warm compresses, anti-inflammatory medications like ibuprofen, and leg elevation are standard first-line approaches. In most cases, this type does not lead to serious complications. However, if symptoms worsen, spread, or are accompanied by swelling of the entire limb, further evaluation is crucial. Your healthcare provider may order an ultrasound to rule out a deeper clot.
9. Prevention Strategies Can Make a Real Difference
Preventing phlebitis is often more effective than treating it after it develops. A comprehensive scoping review identified various nursing interventions for preventing and treating phlebitis associated with peripheral venous catheters, including regular site rotation and proper catheter care. Outside the hospital, staying physically active helps keep blood flowing through your veins. Avoiding prolonged periods of sitting or standing, staying hydrated, and wearing compression stockings during long travel can all reduce your risk significantly.
10. Know When Phlebitis Needs Urgent Attention
While many cases of phlebitis are mild, certain warning signs demand immediate medical attention. High fever, rapidly spreading redness, severe swelling of an entire limb, or difficulty breathing could indicate complications like a blood clot or infection entering the bloodstream. Phlebitis near the junction of superficial and deep veins also carries a higher risk of deep vein thrombosis. Do not hesitate to seek emergency care if your symptoms escalate quickly. Early intervention can prevent a manageable condition from becoming a medical emergency.
Phlebitis is common, but it does not have to catch you off guard. By recognizing the early signs, understanding your personal risk factors, and communicating openly with your healthcare team, you can take meaningful steps to protect your vein health. If you notice any symptoms of vein inflammation, schedule an appointment with your doctor to get a proper evaluation and personalized care plan.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making health decisions.