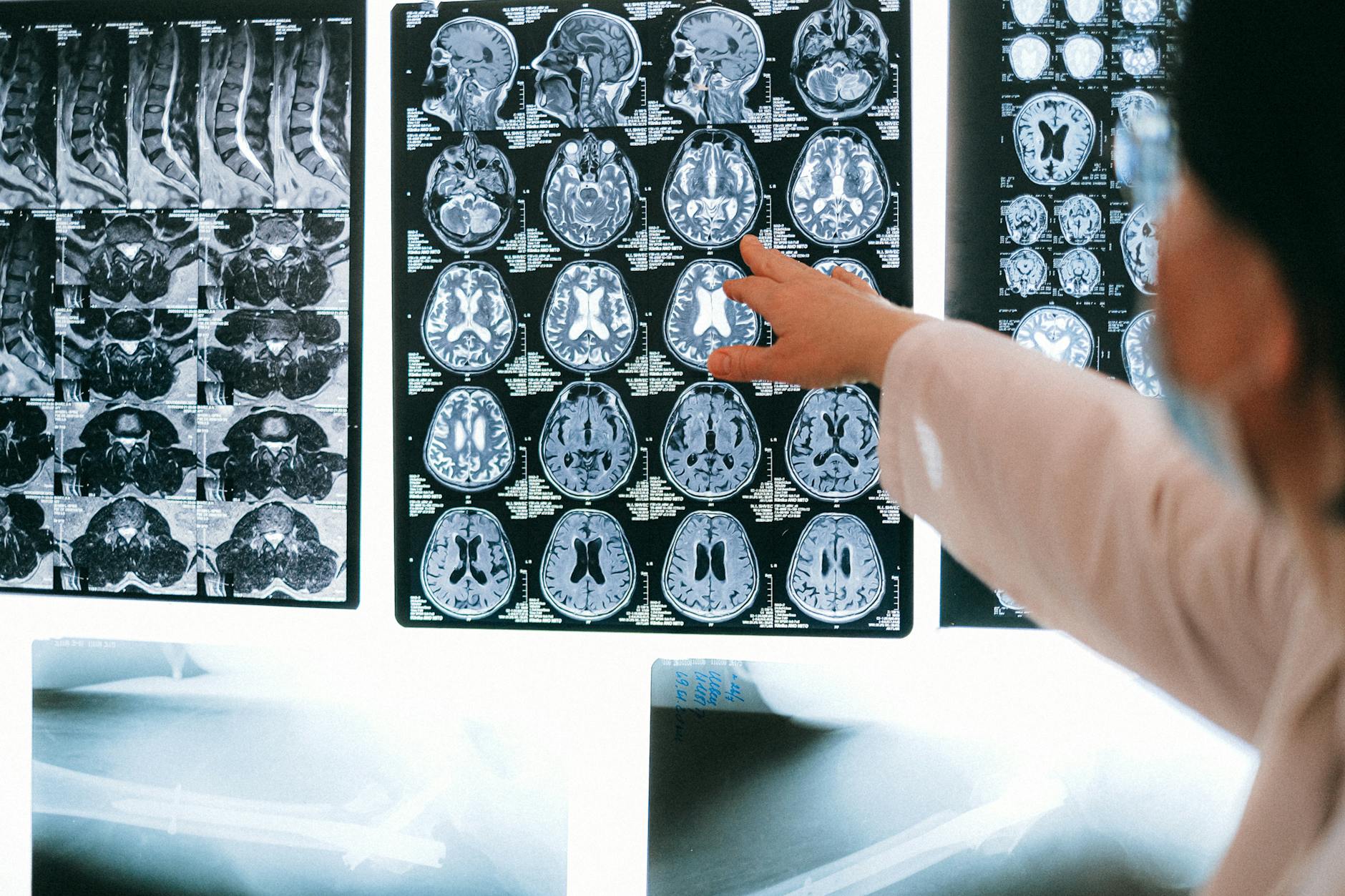
My Tuesday afternoon clinic is mostly people trying to understand why their memory feels muddy or why their left hand suddenly refused to hold a coffee cup. They come in terrified of Alzheimer’s, but the MRI tells a very different story about the tiny vessels feeding their brain. The plumbing is failing long before the tissue dies.
1. The subtle drift of the right eye
You learn in medical school to look for facial drooping. What I actually see in the clinic is a patient fighting to keep their gaze fixed on my nose. Last month a man walked in complaining of sinus pressure. “My face just feels heavy on one side today,” he said. His right eye drifted outward every time he blinked. General practitioners often miss this because they are rushing through a fifteen-minute slot to check blood pressure. But that ocular drift is a massive red flag. It tells me a microvascular event is unfolding right now in the brainstem. The CT scan merely confirmed what his eye had already announced. We admitted him immediately.
2. White matter hyperintensities are not normal aging
Most articles will tell you that finding bright spots on a brain MRI is just a routine part of getting older. That framing misses the point. Radiologists call them white matter changes. I call them tiny scars from years of high blood pressure hammering the delicate microvessels deep in the brain. They are silent strokes. The patient feels nothing when they happen. You just slowly lose your sharp edges. A woman brought her husband in recently because he could no longer calculate tip percentages at restaurants. He was an accountant. In the journal Stroke, Iadecola and colleagues outlined in 2017 how these exact structural vascular shifts slowly degrade the blood-brain barrier. Hypertension drives the damage relentlessly. (You see the effects clearly in the frontal lobes long before memory actually fails.) Patients read their radiology reports and ask me if they have dementia. The truth is their brain tissue is perfectly fine. The blood supply simply stopped delivering oxygen to the wiring.
3. The morning dizziness lie
People wake up dizzy and blame their inner ear or dehydration. They buy supplements. They drink water. But morning vertigo in a sixty-year-old with a history of smoking is a vascular warning until proven otherwise.
The arteries at the back of the neck are simply narrowing.
Blood pools when you lie flat. Then it struggles to push upward against gravity when you stand.
4. The transient ischemic attack that nobody notices
Why do we ignore temporary weakness? Because the human brain is wired to dismiss temporary problems as flukes. A patient sat across from me yesterday and casually mentioned a terrifying event. “I dropped my keys and couldn’t figure out how to pick them up for about ten minutes,” she recalled. She went to sleep instead of the emergency room. By morning her hand worked perfectly fine again. Textbook descriptions make a TIA sound like a dramatic lightning strike of paralysis. In practice it is usually a bizarre moment of clumsiness that resolves before anyone panics. That temporary blockage was a free warning shot from your carotid artery. The next clot will not dissolve on its own.
5. We are seeing it in younger patients now
Ten years ago I rarely ordered a carotid ultrasound for anyone under sixty. Now my schedule is packed with forty-year-olds experiencing unexplained cognitive fog and visual changes. The demographics of cerebrovascular disease are shifting rapidly. A 2019 analysis in the Journal of the American Heart Association by George and colleagues documented a steep increase in event rates among adults aged 35 to 64. I see this reality every week. These younger patients do not have decades of plaque buildup. They have immense chronic stress, poor sleep architecture, and metabolic syndrome that inflames the endothelial lining of their vessels. They come in worried about early-onset Alzheimer’s. I have to explain that their memory issues stem from their fast-food diet and untreated sleep apnea starving their brain of oxygen. The damage accumulates quietly. You cannot feel an artery hardening. You only notice the downstream effects when the plumbing finally struggles to meet the demand of a busy workday.
6. Blood pressure medication is brain protection
Patients hate taking pills. They negotiate with me constantly to stop their lisinopril because they feel fine. I try to explain that we are not treating a number on a cuff. We are protecting the fragile capillaries inside their skull from bursting under microscopic pressure waves. If they could see the micro-hemorrhages on the scans, they might… Well, you can only lead a horse to water.
7. The mystery of small vessel disease
We map the big arteries beautifully. Surgeons can stent a blocked carotid with incredible precision. But the tiny arterioles branching deep into the gray matter remain a frontier we barely grasp. I have to admit that we do not fully understand why some people develop severe small vessel disease despite perfect cholesterol and normal blood pressure. Genetics clearly play a role. A recent special issue of the Journal of Clinical Medicine detailed how artificial intelligence is finally helping us model these microscopic networks. Until those tools reach my clinic, I rely on clinical intuition. I watch how a patient walks down the hallway. A slightly widened stance or a hesitant turn often reveals small vessel damage long before the patient complains of any physical symptoms.
8. Depression that arrives out of nowhere
A seventy-year-old with no psychiatric history suddenly stops caring about their garden. The family assumes it is just situational sadness or grief. I look at their brain imaging and see severe vascular changes in the basal ganglia. We call this vascular depression. The emotional circuits are physically deteriorating because their blood supply is choked off. Treating them with standard antidepressants rarely works. You have to fix the underlying vascular disease. We adjust their statin. We push them to walk daily to force collateral blood flow. Sometimes the mood lifts once the brain gets the oxygen it demands.
9. The silent impact on swallowing
Families notice the memory loss first. They rarely notice the coughing during dinner. Silent aspiration is a hallmark of progressive cerebrovascular disease. The cranial nerves controlling the throat lose their synchronized timing because the motor cortex is slowly starving. Food particles slip past the vocal cords into the lungs. The patient develops a low-grade pneumonia that nobody can explain. I always offer my patients a glass of water during the exam. I listen to the acoustic quality of their voice after they swallow. A wet, gurgly voice tells me more about their vascular health than a dozen blood tests. The brainstem is struggling to orchestrate a basic survival reflex.
10. The myth of full recovery
A stroke is a brain attack. When tissue dies, it stays dead. We try to train the surrounding neurons to take over the lost functions. Sometimes physical therapy works beautifully. Often it hits a wall. I sit with families who expect their father to return to his baseline self after a major middle cerebral artery occlusion. They wait for a miracle. I have to look them in the eye and tell them this is the new baseline.
Monitor your blood pressure at home twice a week, because the clinic readings are never the whole truth. What happens in those tiny vessels today becomes your cognitive reality in ten years.
Medical Disclaimer: This article is for informational purposes only and does not constitute professional medical advice. Always consult a qualified healthcare professional before making changes to your health routine.