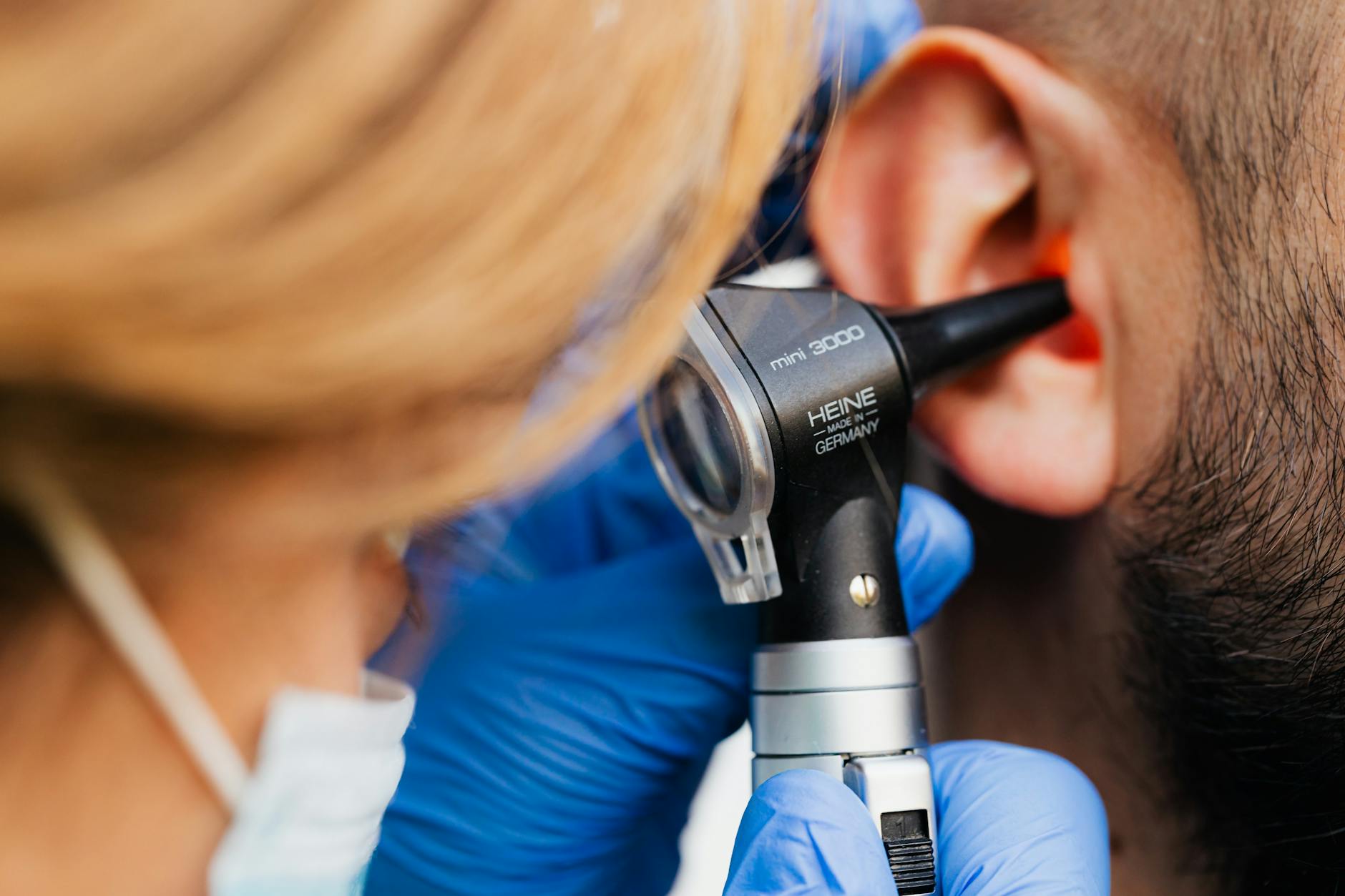
I usually hear them before I see them in the clinic hallway. They grip the doorframe with white knuckles, walking like the floor is pitching on high seas. A vestibular crisis strips away your basic orientation to gravity.
1. The Invisible Earthquake
Before I even touch an otoscope, I watch how they sit down. They freeze their neck. Moving the head accelerates the hallucination of movement, so they guard it fiercely. “It feels like my brain is sliding out of my skull,” a woman told me last Tuesday. That’s labyrinthitis talking. The inner ear is a dark, fluid-filled cave. When a virus inflames the vestibulocochlear nerve, that pathway starts firing garbage data to the brainstem. Your eyes tell you the room is still. But your inner ear screams that you’re spinning at thirty miles an hour. The brain panics. It triggers the vagus nerve, emptying your stomach. You spend three days clutching the bathroom tiles (we call this the acute phase, though it feels like an eternity). I’ve seen grown men weep from the sheer exhaustion of trying to stay upright in a chair. We check for a stroke first. We always do. Once we rule out a cerebellar bleed, we’re left with a tiny, swollen nerve bundle deep inside the temporal bone. There isn’t a magic pill to instantly shrink it. The emergency room will give you meclizine to sedate the vestibular system, but that only dulls the edge. You are still trapped in a body that thinks it’s constantly falling.
2. The Amoxicillin Reflex
General practitioners miss this constantly. A patient complains of dizziness and ear pressure. The doctor glances at a slightly red eardrum and writes a prescription for antibiotics. But the vast majority of these cases are viral vestibular neuritis. Antibiotics do absolutely nothing for a swollen nerve. You’re just nuking your gut flora while the dizzy spells continue unabated.
3. The Middle Ear Spillover
Sometimes the barricade fails. A standard middle ear infection builds up pressure against the round window, which is the porous membrane separating the middle cavity from the inner chamber. Bacterial toxins seep across that boundary. A 2021 review in the Journal of Clinical Medicine noted that 34.9% of acute otitis media patients had inner ear diseases. Half of those people developed worse complications. The labyrinth is supposed to be a sterile sanctuary. When pus and fluid press against that membrane, local inflammation triggers a sympathetic reaction in the cochlea. You get high-frequency hearing loss. Not because bacteria are swimming in the fluid, but because the toxic byproducts of the fight next door are poisoning the delicate hair cells.
4. Textbook Dizziness Fails the Clinic Test
Most articles will tell you an inner ear infection causes vertigo. That framing misses the point. Vertigo is just a word. What does it actually feel like? It’s rarely a clean, carousel-like spinning motion. In the exam room, the presentation is chaotic. Patients report a sudden drop, a pulling sensation to the left, or the floor tilting like a funhouse. They stagger. They can’t read a text message because the letters bounce. Textbooks describe a neat, isolated vestibular deficit. Reality is a messy cascade of visual mismatch and autonomic panic. Why does your heart race? Because your brain interprets the conflicting sensory input as neurotoxin poisoning. It literally thinks you ate a bad berry and is trying to purge the poison.
5. The Silent Immune Highway
We used to think the labyrinth was entirely walled off from the rest of the body. An immune-privileged vault. That was wrong. The inner ear actively talks to your systemic immune system. A 2022 paper in Frontiers in Immunology demonstrated how inflammatory cells enter from spiral ligament venules during an attack. White blood cells squeeze through microscopic blood vessels to hunt the virus. The swelling you experience is friendly fire. Your own body inflames the delicate tissues to trap the pathogen. That collateral damage is what makes you deaf and off-balance. The nerve itself isn’t the virus’s primary target. It’s just caught in the crossfire of a microscopic warzone.
6. The Meningitis Backdoor
The anatomy has a fatal flaw. The cochlear aqueduct connects the inner ear directly to the cerebrospinal fluid. In severe cases of bacterial meningitis, pneumococci invade the inner ear through this channel. The bacteria spread rapidly through the perilymphatic spaces. This is why absolute deafness frequently follows meningitis. The infection breaks in through the basement window.
7. The Tell-Tale Eye Flick
“I’m not dizzy, my eyes are just vibrating.” A young carpenter said that to me last month, perfectly describing nystagmus. When your vestibular nerve is damaged on one side, your eyes drift slowly toward the bad ear, then snap back violently to the center. Over and over. I don’t need an MRI to diagnose you in that exact moment. I just ask you to follow my finger. The direction of the eye snap tells me exactly which side is infected. The brain is desperately trying to stabilize your gaze while receiving corrupted data from the ear. It’s a reflex you can’t fake. And you can’t stop it, either.
8. The Hearing Recovery Lottery
Labyrinthitis takes your hearing. Vestibular neuritis just takes your balance. If the inflammation hits the entire labyrinth, you’ll notice a sudden muffling in the affected ear. This is often accompanied by a high-pitched ringing that sounds like a dying fluorescent bulb. We treat this aggressively with high-dose oral steroids. The goal is to shut down the swelling before it permanently scars the cochlear hair cells. A 2023 retrospective study in the Journal of Otolaryngology found high rates of complete hearing recovery across multiple treatment protocols, hovering around sixty percent. But why do the other forty percent lose their hearing forever? We honestly don’t fully understand the mechanism yet. Two patients can have the exact same viral load, take the exact same dose of prednisone, and have wildly different outcomes. One gets their hearing back in two weeks. The other needs a hearing aid for the rest of their life. It’s the hardest conversation I have to have in the clinic, telling someone their sudden deafness is likely permanent. We map the audiogram, watch the flat line in the high frequencies, and hope the nerve wakes up. Sometimes it just refuses. The cellular damage crosses a threshold we simply cannot reverse.
9. The Brain’s Recalibration
The damaged nerve rarely heals back to one hundred percent. The viral attack kills off delicate neural fibers. Yet, most people stop feeling dizzy after a few weeks.
Your brain simply learns to ignore the broken ear.
This process is called vestibular compensation. The central nervous system rewires itself to rely heavily on your vision, along with the proprioceptive sensors in your ankles and joints. It patches the software to hide the hardware failure. But if you walk into a pitch-black room, stripping away your visual anchors, the dizziness comes rushing back. You stumble. The compensation relies on light and physical touch to maintain the illusion of balance.
10. The Lingering Ghost
Months after the acute infection clears, you might still feel a sudden wave of nausea when you turn your head too fast in the grocery store aisle. Looking at busy geometric patterns can trigger a strange sweating. The brain gets tired. When you’re stressed, sleep-deprived, or fighting off a mild cold, that neural software patch we talked about starts to glitch. The compensation slips. You aren’t infected again. You’re just experiencing the residual shadow of the original damage. The inner ear never forgets the insult. The scar tissue remains, quietly misfiring in the dark, waiting for your brain to drop its guard.
A sudden loss of balance paired with hearing changes is a neurological emergency until proven otherwise. Bypass the urgent care clinic and go straight to an emergency room for a thorough evaluation.
Medical Disclaimer: This article is for informational purposes only and does not constitute professional medical advice. Always consult a qualified healthcare professional before making changes to your health routine.