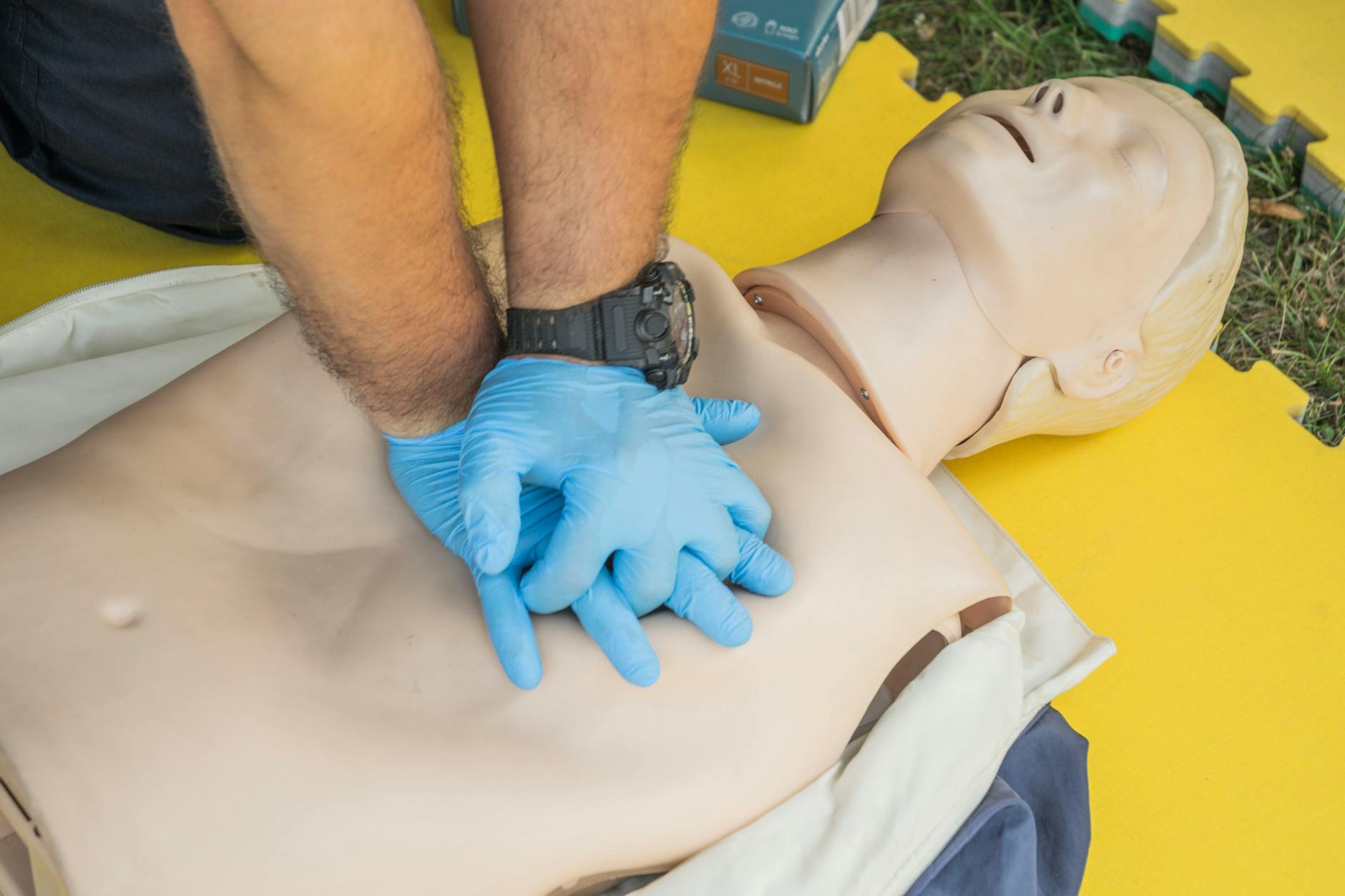
Every year, hundreds of thousands of people experience out-of-hospital cardiac arrest, and bystander response in the first few minutes can mean the difference between life and death. Agonal breathing is one of the most commonly misidentified signs during these emergencies, often causing witnesses to delay calling 911 or starting CPR. Understanding this reflexive gasping pattern could genuinely help you save someone’s life.
1. It Is Not Normal Breathing
Agonal breathing is a series of irregular, labored gasps that occur when the brain is severely deprived of oxygen. Unlike normal respiration, these gasps are not effective at delivering oxygen to the body. They often sound like snorting, gurgling, or moaning and may happen only a few times per minute. Many bystanders mistake agonal breathing for a sign that someone is still breathing adequately. This misinterpretation is one of the most dangerous mistakes during a cardiac emergency. If someone collapses and you hear unusual gasping, treat it as a cardiac arrest and begin CPR immediately.
2. It Occurs in Nearly Half of Cardiac Arrests
Research suggests that agonal breathing is far more common than most people realize. According to PubMed, agonal respirations occur in approximately 40% of out-of-hospital cardiac arrests. They are particularly associated with witnessed arrests and cases involving ventricular fibrillation. This means that if you ever witness someone collapse from a cardiac event, there is a strong chance you will encounter these abnormal gasps. Knowing what to expect ahead of time can help you respond faster and more confidently when every second counts.
3. It Is a Brainstem Reflex
Agonal breathing originates from the brainstem, the most primitive part of the brain responsible for basic survival functions. When the heart stops pumping blood, the higher brain regions shut down quickly, but the brainstem can continue firing signals briefly. These signals trigger the characteristic gasping movements. The gasps are involuntary and do not indicate consciousness or awareness. Think of it as the body’s last-ditch effort to restart oxygen flow. Understanding this mechanism helps explain why agonal breathing should never be confused with purposeful breathing.
4. It Can Actually Be a Positive Sign
While agonal breathing is alarming to witness, clinical evidence shows it may signal a better chance of survival. A study published in PubMed found that agonal breathing at hospital arrival was significantly associated with improved neurological outcomes and higher survival rates at one month. This is likely because agonal gasps indicate the arrest happened recently and the brain has not yet suffered irreversible damage. The presence of these gasps suggests a narrow but critical window for effective resuscitation. If you witness them, act fast because the prognosis may still be favorable.
5. It Sounds Different Than You Might Expect
Most people picture gasping when they think of breathing emergencies, but agonal breathing can take many forms. It may sound like loud snoring, sporadic grunting, or even a strange gurgling noise. Some people describe it as sounding like the person is trying to breathe through water. The intervals between gasps are typically long and irregular. A person might take one gasp, then nothing for 10 to 20 seconds, then another gasp. These unpredictable patterns make it easy to assume the person is breathing when they actually need immediate help.
6. It Is a Major Reason Bystanders Delay CPR
Studies indicate that agonal breathing is one of the top reasons bystanders hesitate to start chest compressions. When people see someone gasping, they often believe the person is still alive and breathing on their own. This confusion leads to critical delays in calling emergency services and beginning CPR. Research published in PubMed demonstrated that specific training on recognizing agonal breathing significantly improved diagnostic accuracy and CPR initiation rates. The takeaway is clear: public education about this phenomenon could save thousands of lives each year.
7. It Can Happen Within Seconds of Cardiac Arrest
Agonal breathing typically begins within moments of the heart stopping. Once blood flow to the brain ceases, the brainstem starts producing these gasping reflexes almost immediately. In many cases, the gasps start before the person even hits the ground. This rapid onset is part of why witnesses often feel confused about what is happening. They see someone fall and hear breathing sounds, so they assume the person is conscious. Recognizing that gasping can begin instantly after cardiac arrest helps reframe the urgency of the situation.
8. It Usually Stops Within Minutes
Agonal breathing is a temporary phenomenon. Without intervention, these gasps typically cease within a few minutes as the brainstem loses its remaining oxygen supply. Once the gasping stops entirely, the window for successful resuscitation narrows dramatically. This brief timeline underscores why immediate action is so important. Every minute without CPR reduces the chance of survival by roughly 7 to 10 percent. If you notice someone gasping abnormally, do not wait to see if their breathing improves on its own. Start chest compressions and call for help right away.
9. 911 Dispatchers Are Trained to Identify It
Emergency dispatchers receive specialized training to recognize descriptions of agonal breathing over the phone. If you call 911 and describe someone making occasional gasping or snoring sounds after collapsing, a trained dispatcher should guide you to begin CPR. However, communication gaps still occur. Callers sometimes describe the sounds in ways that obscure the seriousness of the situation. Being specific about what you see and hear is essential. Tell the dispatcher the person is unresponsive and making abnormal gasping sounds so they can provide the right instructions quickly.
10. Learning to Recognize It Could Save a Life
Perhaps the most important fact about agonal breathing is that recognizing it is a learnable skill. CPR training courses increasingly include education about agonal respirations and how they differ from normal breathing. Many programs now use audio and video examples to help trainees identify the sounds. Community-based training initiatives have shown measurable improvements in bystander response rates. You do not need a medical degree to make a difference in a cardiac emergency. Taking a certified CPR course that covers agonal breathing recognition is one of the most impactful health decisions you can make for your community.
Agonal breathing is a misunderstood but critically important sign of cardiac arrest that affects nearly half of all out-of-hospital cases. By learning to recognize these abnormal gasps and responding with immediate CPR, you could dramatically improve someone’s chance of survival. Consider enrolling in a CPR course and sharing this knowledge with your friends and family.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making health decisions.