Pleural effusion is a condition that affects well over a million Americans annually, yet many people have never heard of it until they or a loved one receive a diagnosis. Understanding what is pleural effusion — and why it happens — can help you recognize warning signs early and have more informed conversations with your doctor. Here’s what the science says about this common but often misunderstood condition.
1. It’s a Fluid Buildup Between the Lung Linings
At its core, pleural effusion is the abnormal accumulation of fluid in the pleural space. This is the thin, fluid-lined cavity that sits between the two layers of tissue surrounding your lungs. Normally, a small amount of fluid exists here to help your lungs glide smoothly as you breathe. When too much fluid collects, it can compress lung tissue and make breathing difficult. According to the NCBI/NIH, this buildup occurs within the pleural space and can range from mild to severe. If you experience unexplained shortness of breath, talk to your healthcare provider about whether fluid around the lungs could be the cause.
2. There Are Two Main Types
Not all pleural effusions are alike. Doctors classify them into two broad categories: transudative and exudative. Transudative effusions happen when fluid leaks into the pleural space due to pressure changes. Heart failure is the most common cause. Exudative effusions result from inflammation, infection, or cancer that damages the pleural lining. As the Cleveland Clinic explains, this classification helps doctors pinpoint the underlying cause and guide treatment decisions. Knowing the type matters because it shapes the entire treatment plan.
3. Heart Failure Is the Leading Cause
Congestive heart failure tops the list of conditions that lead to pleural effusion. When the heart can’t pump blood efficiently, pressure builds in the blood vessels around the lungs. This forces fluid into the pleural space. Research published in PubMed Central identifies congestive heart failure, cancer, pneumonia, and pulmonary embolism as the most common causes. Managing heart health through diet, exercise, and medication may help reduce the risk of developing this complication. Always work with your cardiologist if you have heart-related concerns.
4. Infections Can Trigger It Too
Pneumonia and other lung infections are significant contributors to pleural effusion. When bacteria or viruses infect the lungs, the resulting inflammation can cause fluid and pus to accumulate in the pleural space. This specific type is often called a parapneumonic effusion. In severe cases, the fluid can become infected itself, creating a condition known as empyema. Tuberculosis is another infectious cause, particularly in developing countries. Seeking prompt treatment for respiratory infections is one practical way to lower your risk of this complication.
5. Cancer Is a Serious Underlying Cause
Malignant pleural effusion occurs when cancer cells invade the pleural lining. Lung cancer and breast cancer are the most frequently associated types. Lymphoma and mesothelioma can also be responsible. The presence of a malignant effusion often signals advanced-stage disease. Clinical evidence shows that these effusions tend to recur even after drainage. Treatment focuses on managing symptoms and addressing the underlying malignancy. If you have a cancer diagnosis and notice new breathing difficulties, report them to your oncologist immediately.
6. Symptoms Can Be Subtle at First
Small pleural effusions sometimes produce no symptoms at all. Many people discover them incidentally during imaging for another issue. As fluid accumulates, the most common symptom is shortness of breath, especially during physical activity. A dry, persistent cough and chest discomfort that worsens with deep breathing are also typical signs. Some people experience a sharp, stabbing chest pain called pleuritic pain. Because these symptoms overlap with many other conditions, they can be easy to dismiss. Pay attention to any new or worsening respiratory symptoms and bring them up at your next appointment.
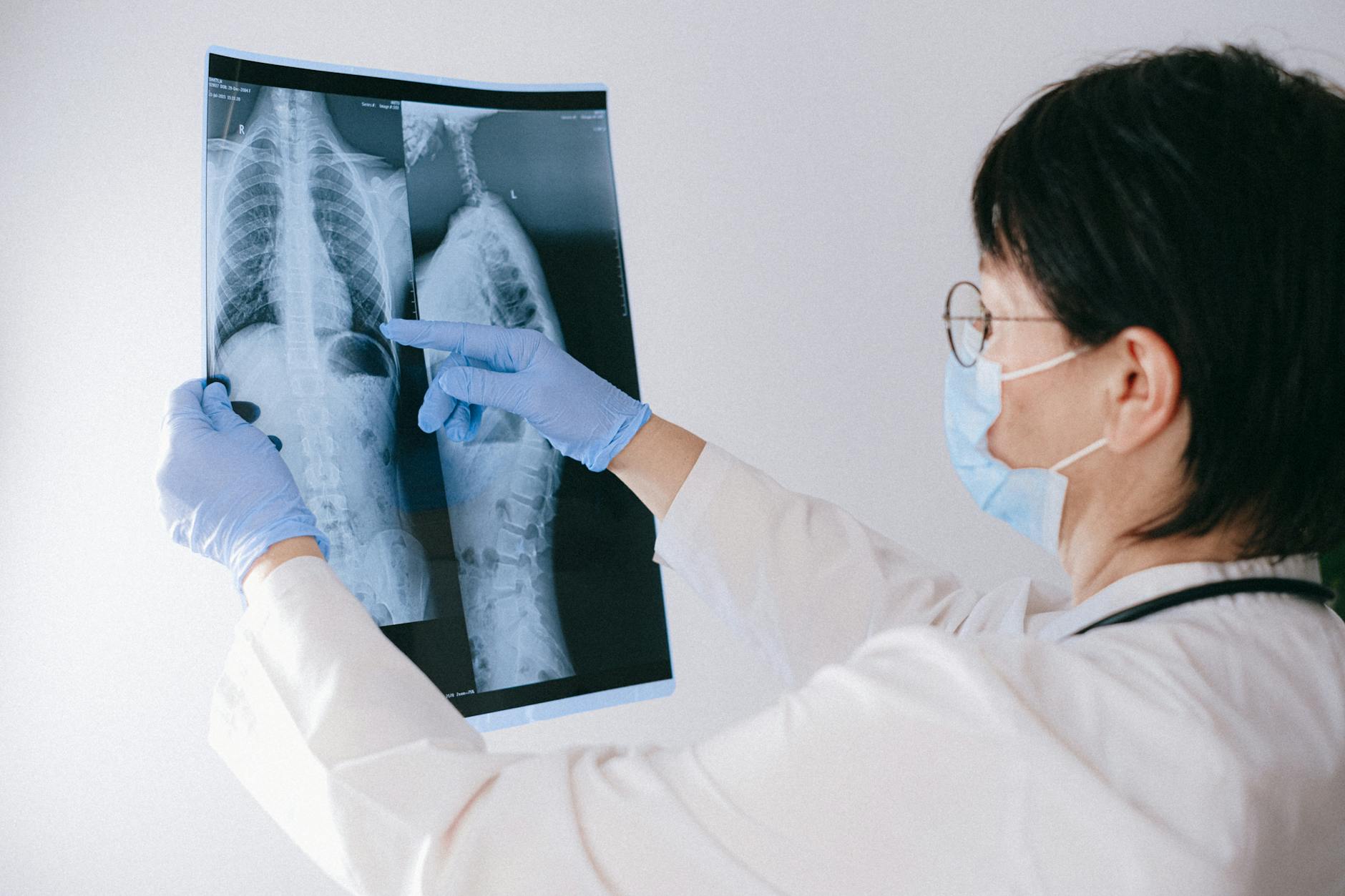
7. A Chest X-Ray Is Usually the First Step
Diagnosing pleural effusion typically starts with a standard chest X-ray. Even a modest amount of fluid can appear as a white, hazy area at the base of the lung. Ultrasound is another valuable tool that helps doctors see exactly where the fluid sits. CT scans provide more detailed images and can reveal potential causes like tumors or infections. Once fluid is identified, doctors often perform a thoracentesis — inserting a needle to draw out a sample for analysis. This fluid analysis is critical for determining whether the effusion is transudative or exudative.
8. Thoracentesis Serves Double Duty
Thoracentesis is both a diagnostic and therapeutic procedure. During the process, a doctor inserts a thin needle through the chest wall into the pleural space. They can remove fluid for laboratory testing to identify the cause. At the same time, draining excess fluid often provides immediate relief from breathing difficulties. The procedure is generally well-tolerated and performed under local anesthesia. Most patients feel noticeably better once the fluid pressure on their lungs is reduced. Ask your doctor what to expect before and after the procedure if it’s been recommended for you.
9. Recurrence Is Common Without Treating the Root Cause
One of the more frustrating aspects of pleural effusion is its tendency to come back. Draining the fluid addresses the symptom but not the underlying problem. Studies indicate that effusions caused by cancer or chronic heart failure are particularly prone to recurrence. For recurring cases, doctors may recommend pleurodesis, a procedure that seals the pleural layers together to prevent fluid from re-accumulating. Another option is placing an indwelling pleural catheter for ongoing drainage at home. Working closely with your medical team to manage the root condition is the most effective way to reduce repeat episodes.
10. Early Detection Improves Outcomes Significantly
Catching pleural effusion early can make a meaningful difference in treatment success and quality of life. Small effusions are easier to manage and less likely to cause complications like lung collapse or infection. People with chronic conditions such as heart failure, liver disease, or kidney disease should be especially vigilant about respiratory changes. Regular checkups and honest communication with your doctor are your strongest tools. Research suggests that early intervention helps prevent the progression to more complicated and harder-to-treat stages. Don’t wait for symptoms to become severe before seeking evaluation.
Pleural effusion is a condition with many possible causes, ranging from heart failure to infection to cancer. Understanding these key facts can empower you to recognize symptoms, ask the right questions, and seek timely medical care. If you or someone you know is experiencing unexplained breathing difficulties or chest discomfort, schedule a visit with a healthcare provider as soon as possible.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making health decisions.