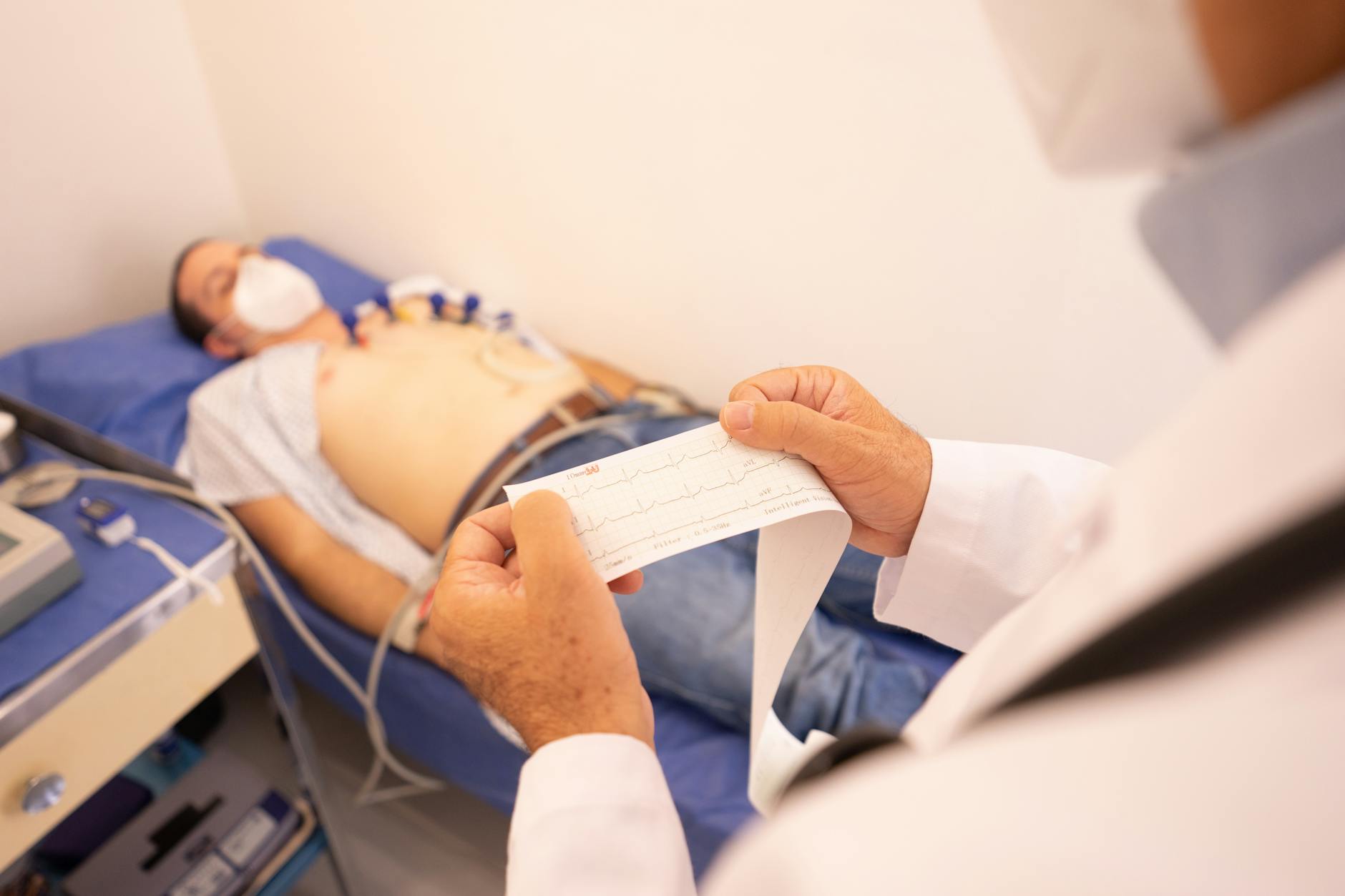
The printout slides out of the machine and spits out an automated interpretation in bold red letters. Most people panic immediately when they see the word block printed next to their own name. I’ve spent a decade walking into exam rooms to talk people down from that ledge.
1. The word block is a terrible metaphor
Patients hear left bundle branch block and picture a clogged pipe. “Is it plaque, Doc? Am I having a heart attack right now?” That isn’t what’s happening. The heart has electrical wires. One of them is just taking a fraction of a second longer to fire. It’s a detour. Not a wall.
2. The hunt for the phantom baseline
This is where triage breaks down. A patient goes to a walk-in clinic for a chest cold and the physician assistant runs a routine EKG. It shows the abnormality. The GP sees the squiggly lines widening out and immediately sends the patient to the emergency room to rule out an active infarction. I see this twice a month. The emergency room runs troponin levels, keeps the patient overnight, and frightens everyone involved. But what gets missed at the GP level versus the specialist level is the relentless hunt for context. I don’t care what your EKG looks like today nearly as much as I care what it looked like five years ago. If you had a left bundle branch block in 2018 and you have it today, my blood pressure stays perfectly normal. If this is a brand new change, the conversation shifts entirely. We aren’t looking at an anatomical quirk anymore. We’re looking at a changing environment inside the cardiac muscle. We have to figure out what insulted the left ventricle enough to damage the wiring. Which could be a virus, or micro-vessel disease, or… we just need more tests.
3. The sluggish left ventricle
The left ventricle is your heart’s main pumping chamber. When the electrical signal hits a delay, the walls of that chamber don’t squeeze at the exact same time. It creates a slight wobble. Over years, that uncoordinated contraction can wear the muscle out. In the Journal of the American Heart Association, a 2018 paper by J.A. Smiseth detailed how this uncoordinated ventricular contraction leads to left ventricular contractile inefficiency. The muscle works harder just to push the exact same volume of blood.
You might not feel it right away, but the heart knows.
4. The quiet fatigue
I can sometimes spot the downstream effects before the tech even places the twelve leads on your chest. A woman in her sixties sat on my table last year and sighed heavily just taking off her coat. She said, “I just feel like I’m walking through wet cement lately.” She thought she was just aging. I looked at her neck veins and noticed a faint, rapid pulsation. Her ankles were slightly puffy above her socks. The textbook presentation of heart failure from a left bundle branch block involves overt shortness of breath and fluid in the lungs. In the exam room, it’s much quieter. It’s a slow fade in stamina that patients write off as getting older until the EKG gives us the actual reason.
5. Can a healthy heart have a block?
Yes, and it happens more than you think. You can have completely clear arteries and perfect cholesterol and still develop a left bundle branch block. The electrical system ages independently of the plumbing. Sometimes the wires just fray.
6. The ultrasound dictates the next move
You can’t diagnose the physical strength of a heart from an electrical printout. You need an echocardiogram. This uses sound waves to watch the muscle squeeze in real time. We’re looking for the ejection fraction. If your ejection fraction is dropping, the block is no longer a harmless bystander. In a 2020 review by F. Gentile, researchers demonstrated how even in structurally normal hearts, this delay is associated with increased risk of heart failure. We watch that percentage like a hawk. If it dips below thirty-five percent, we stop watching and start intervening.
7. The shape shifts
The heart is highly adaptable (sometimes to its own detriment). When the electrical sequence is off, the physical shape of the ventricle actually starts to change to compensate. We call this cardiac remodeling. According to a 2019 paper by M. Vernooy, a left bundle branch block causes sequential ventricular activation that alters the actual shape and workload of the heart. It gets rounder. Less efficient. The walls thin out.
8. The biventricular upgrade
Most articles will tell you a pacemaker is the inevitable end road for this condition. That framing misses the point entirely. A standard pacemaker just keeps the heart from beating too slowly. It does nothing to fix the uncoordinated wobble of a left bundle branch block. If we intervene, we use cardiac resynchronization therapy. We thread three wires into the heart instead of two. We force the left and right sides to squeeze at the exact same millisecond again. The muscle remembers what it feels like to work properly.
9. Masking the real emergencies
There is an incredibly frustrating side effect of having this exact electrical pattern permanently stamped onto your medical record. It obscures our view of everything else that might be going wrong. If you come into the emergency room with sudden chest pain and a normal EKG, we can spot a heart attack immediately. The ST segments elevate. It’s obvious. Everyone rushes into action. But a left bundle branch block wildly distorts the ST segments at baseline. It throws heavy static over the entire reading. Decades ago, doctors created complex scoring systems to try and read through the static. We’re still debating in hospital hallways how well those criteria actually work in real time. I will admit the cardiology community doesn’t have a flawless system for catching acute ischemia in the presence of a preexisting block without turning to blood tests or an immediate angiogram. It forces my hand. I have to be far more aggressive with invasive testing when a patient with this history complains of chest tightness. I can’t trust the paper printout anymore. The static hides the fire. We end up admitting people just to be absolutely sure we aren’t missing a blocked artery hiding behind the frayed wiring.
10. The asymptomatic majority
“I wouldn’t have even known I had a heart problem if I didn’t need clearance for my knee surgery.” A patient told me that yesterday. He’s right. Millions of people walk around with this electrical delay and never develop a single symptom. Their ejection fraction stays normal. Their heart shape never changes. We do an ultrasound every year, we shake hands, and I tell them I’ll see them in twelve months. The hardest part of the diagnosis is living with the lingering knowledge that your heart is electrically imperfect.
Medical Disclaimer: This article is for informational purposes only and does not constitute professional medical advice. Always consult a qualified healthcare professional before making changes to your health routine.