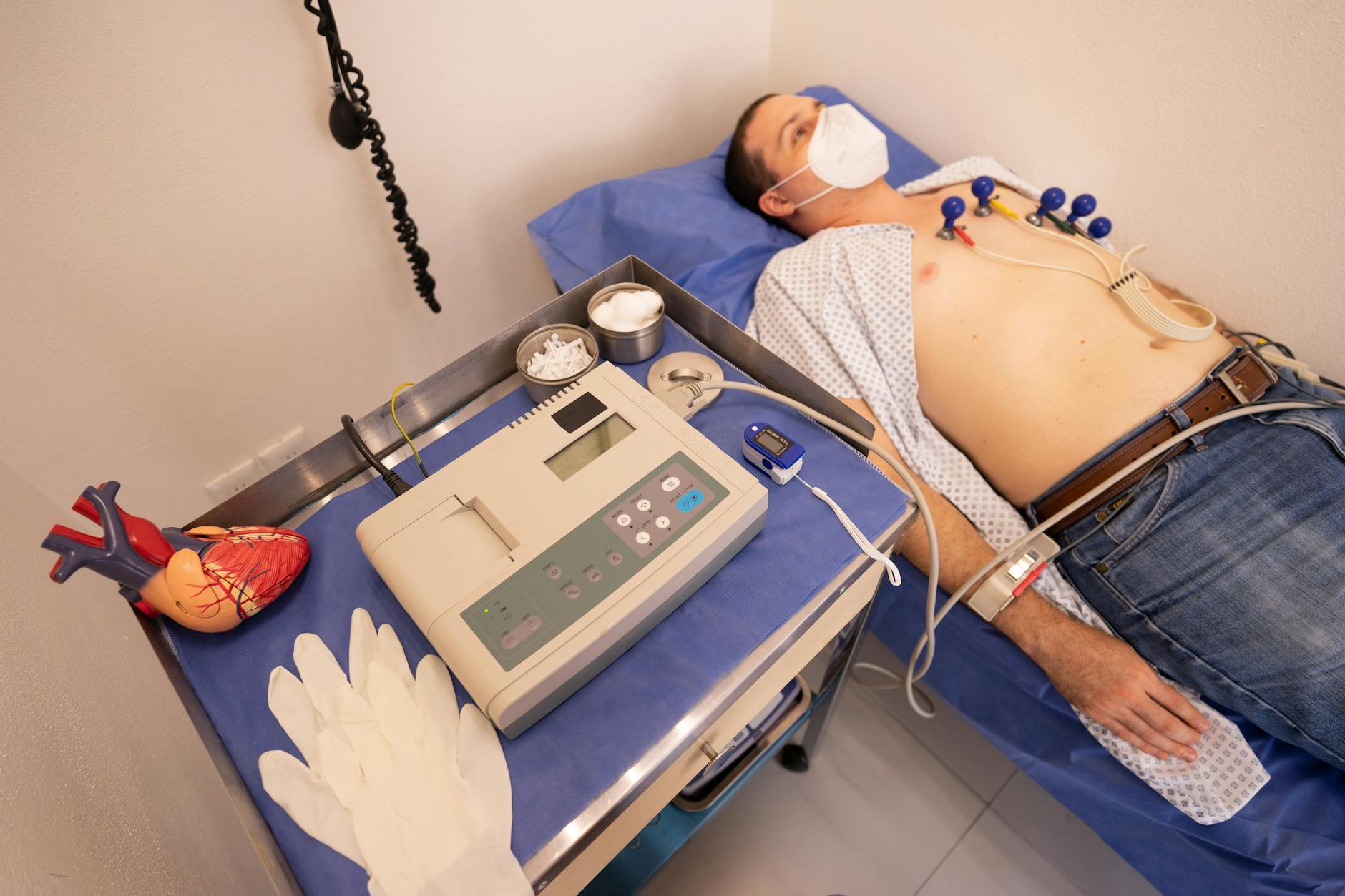
I look at wrist monitors all day long now. People walk into my clinic clutching printouts from their smartwatches, terrified because their pulse dipped to 54 while they slept.
1. The textbook illusion
Most articles will tell you 60 to 100 beats per minute is the golden window. That framing misses the point. The established medical literature defines this as the standard range for a human sitting quietly. But an average is just a mathematical compromise. A general practitioner sees a resting pulse of 95 on an annual physical chart and moves on to the next room. As a cardiologist, I see a resting pulse of 95 in a healthy thirty-year-old and I start wondering about early heart failure or severe deconditioning. We’re trained to look for patterns rather than isolated data points. Patients constantly panic over absolute numbers. Last week a young man sat in my office and said, “My app says my heart is failing because I hit 105 walking to the bathroom.” I had to explain that a heart rate is supposed to accelerate when you demand physical work from your muscles. Textbooks describe sinus tachycardia as a rapid regular rhythm driven by physiological demand. In the exam room, it looks like a terrified accountant staring at his smartwatch while his sympathetic nervous system dumps adrenaline into his bloodstream because his wrist vibrated. A solitary number pulled from a Tuesday afternoon tells me absolutely nothing about your actual cardiovascular risk profile. You have to contextualize the beat.
2. Digestion demands a pulse
Why does your pulse spike after lunch? Your gut needs blood to process that heavy meal. The gastrointestinal tract pulls volume away from your extremities to absorb nutrients. Your heart compensates by pumping a little faster to maintain systemic pressure. People often misinterpret this post-meal flutter as anxiety. It’s just basic plumbing doing exactly what millions of years of evolution designed it to do.
3. Age rewires the baseline
The rhythm you had at twenty won’t be the rhythm you keep at sixty. Electrical pathways in the cardiac tissue slowly fibrose as decades pass. The Journal of Clinical Monitoring and Computing (2024) outlined that the mean ambulatory pulse for men in their fifties sits roughly between 57 and 90 beats. Women run slightly faster, peaking around 92. I watched a fifty-five-year-old woman’s hands trembling slightly as she handed me her intake form, her skin damp, and I knew her thyrotoxicosis was back before the EKG leads even touched her chest. She told me, “It feels like a bird is trapped in my chest.” The monitor confirmed she was sitting at 115. Her age was irrelevant to that specific pathology, but her baseline had shifted over the years. We treat the change.
4. The nocturnal dip
Your body forces you into a state of suspended animation while you sleep. Parasympathetic tone dominates. The vagus nerve clamps down on the sinoatrial node.
This is completely intentional.
(Most marathoners I treat sit around 40 beats per minute in deep sleep). Yet people wake up, check their sleep data, and assume they almost died. The alarm bells ring in their heads. A resting pulse in the mid-forties during REM sleep indicates an efficient cardiovascular system recovering from the day. You want that muscle to rest. If your monitor buzzes to warn you about a low pulse at 3 AM, the monitor is the actual problem.
5. The anxiety feedback loop
Checking your pulse raises your pulse. The simple act of focusing on your chest cavity alerts the brain to a potential threat. Cortisol leaks into the system. The heart accelerates to meet the phantom danger. A population analysis published in 2019 found that while the accepted range is wide, the real-world average resting pulse hovers right around 79 beats per minute. But that number represents people living their lives, not people terrified of their own biology. We still don’t completely understand why two genetically similar people with identical fitness levels can sit at rest twenty beats apart.
6. Premature contractions disguise themselves
Sometimes the rhythm stumbles. You feel a massive thud in your throat. Then you wait for the next beat and it takes too long to arrive. People immediately check their pulse and find the rate has plummeted to 40. They think their heart is failing. What actually happened is an ectopic beat fired early from the lower chambers. The heart paused to reset its electrical grid. That pause feels like an eternity. The subsequent beat is unusually forceful because the chambers had extra time to fill with blood. You feel the compensatory thud and assume the worst, though it usually just means you drank too much coffee or slept poorly. The wearable device only registers the long pause, calculating a falsely low average rate for that minute. The machine lacks nuance. It can’t distinguish between a dangerous conduction block and a harmless premature ventricular contraction. We spend hours reassuring patients that their plumbing is fine and their electrical wiring just had a minor hiccup. You’re feeling the reset mechanism. The rate never actually dropped in a sustained way. It was just a brief interruption in the circuit that fooled the algorithm. The fear that follows usually triggers a rush of adrenaline, which then forces the sinus node to fire rapidly to overcompensate. You end up creating the exact erratic pattern you were terrified of finding in the first place.
7. Hormonal tides
Estrogen and progesterone dictate fluid volume. A woman in her luteal phase will often see her resting pulse climb by five to ten beats. The body is warming up, retaining water, preparing the uterine lining. This mild tachycardia resolves when menstruation begins. There’s no pathology here. It’s just the endocrine system talking to the cardiovascular system.
8. Dehydration shrinks the pipes
Blood is mostly water. When you sweat heavily or forget to drink, your total blood volume drops. The physical pipes shrink. To maintain adequate pressure to the brain, the heart has to cycle that diminished volume much faster. A sudden resting rate of 90 on a hot afternoon is rarely a cardiac event. It’s usually just a plea for fluid. I see this constantly in the summer months. Patients walk into the clinic dizzy, convinced their rhythm is irregular. A liter of saline through an IV drops their pulse back to 65 in twenty minutes.
9. The fitness paradox
Athletes build larger left ventricles. Each contraction pushes a massive stroke volume into the aorta. Because the pump is so efficient, it doesn’t need to beat as often. A resting rate of 45 in a sedentary office worker is a red flag for sinus node dysfunction. That exact same rate in a cyclist is a badge of honor. The broader clinical consensus still labels 60 to 100 as the standard, but fitness obliterates that bell curve. Context dictates the pathology.
10. The threshold for intervention
We don’t treat numbers on a screen. We treat the human sitting on the exam table. If your pulse is 110 and you feel perfectly fine, we might just watch it. If your pulse is 110 and you cannot catch your breath, we intervene immediately. The raw data means very little without the physical symptoms accompanying it. A monitor can’t tell me if your skin is clammy. It can’t tell me if your chest aches. You either have symptoms or you have data. We only medicate the symptoms.
Stop staring at your wrist every time you feel a flutter. Throw the watch in a drawer for a week and see how your chest actually feels.
Medical Disclaimer: This article is for informational purposes only and does not constitute professional medical advice. Always consult a qualified healthcare professional before making changes to your health routine.